Normal View Dyslexic View
Surgical digest
Can recurrent diverticulitis be predicted?
Diverticular disease is a common disorder, and recent guidelines report on new treatment strategies such as non-antibiotic management. Patients with diverticular disease are increasingly being treated as outpatients. In addition, fewer patients are undergoing emergency surgery whereas there is an increase in the use of elective and laparoscopic surgery in the management of diverticulitis. However, several aspects are still controversial. Strong evidence still lacks for the therapeutic management of patients with recurrent episodes of acute diverticulitis or patients with persistent abdominal symptoms after acute attacks. The European Society of Coloproctology (ESCP) guideline committee reviewed the literature and developed the European guidelines for the management of diverticular disease of the colon in 2020. In spite of the existence of several different classifications for diverticulitis, the committee decided neither to create another classification nor to endorse any of the existing ones. Nevertheless, phlegmonous diverticulitis, considered as uncomplicated by most of the classifications, is a matter of concern since it includes about 70% of the patients with acute diverticulitis. This group of patients may be clinically heterogeneous in terms of characteristics or disease evolution, which in some cases might be complicated. Patients at risk that belong to initially uncomplicated stage need to be identified in order to prevent complications and receive the most appropriate medical/surgical treatment.
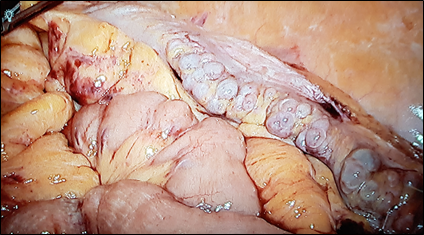
Classically, colonic resection after the second episode of acute diverticulitis has been supported, since any following episodes will respond insufficiently to medical treatment and with higher morbidity and mortality2. Recently, it was reported that 6.8-27.7%3,4 of patients with acute diverticulitis treated conservatively may require surgical intervention due to complicated diverticulitis or persistent symptoms, most of them during the first year of follow-up. In addition, elective sigmoidectomy seems to be related with a better quality of life (QOL) compared with conservative management in patients with recurring diverticulitis and/or ongoing complaints5,6. Nowadays, the main reason to perform elective sigmoid colectomy (Fig 1) in patients with recurrent disease or with ongoing symptoms after an acute episode of diverticulitis is to improve their QOL. In fact, there are many patients in whom initial antibiotic treatment fails, leading to sub-acute / chronic diverticulitis. In these patients the differentiation between sub-acute ongoing diverticulitis which never resolved, i.e. persisting disease, and a true recurrence is very difficult7.
Fig 1. Chronic diverticulitis who underwent emergent colonic resection
Chronic diverticulitis (Fig 1), considered as a true condition for the first time by the ESCP group, occurs when there is colonic wall thickening or chronic inflammation of the mucosa1. It can appear when an acute diverticulitis does not resolve completely, and it can have an important impact on QOL of the patients, causing persistent abdominal symptoms (abdominal pain, bloating) and changes in bowel habit. However, the uncertainty of the evolution of the disease and the lack of clear signs to identify which patients will develop a chronic condition, make the selection of patients and the best moment to advise surgical resection difficult. Colonic resection has been shown to effectively reduce the number of recurrences, but it should be kept in mind that it is a major surgery with potential severe complications1. The distinction between Irritable Bowel Syndrome (IBS) and symptoms related to chronic diverticulitis after an episode of diverticulitis is of utmost importance, because IBS is a functional disorder and should not be treated surgically8. Endoscopy could help in those cases where differential diagnosis is difficult5. It should be noted that after sigmoidectomy, 25% of patients persist with functional symptoms and abdominal pain9.
Immunosuppressed patients deserve special attention. In these patients, the onset of diverticulitis is more aggressive, and more often leads to perforation1. It has been observed that in post-transplant patients the incidence of acute diverticulitis is 1.7%, debuting as complicated acute diverticulitis in 40%, while the incidence of complicated acute diverticulitis in immunocompetent patients is 10%-15%10. Patients with chronic corticosteroid use are at increased risk of urgent surgery at the debut of diverticulitis. Moreover, they present a higher recurrence risk without need of emergent surgery especially in the first year after the index episode 1.
Publications describing predictors of recurrence and/or chronic disease in diverticulitis are scarce11. Drawing a parallel between diverticular disease and inflammatory bowel disease (IBD), it seems that in both diseases, active intestinal inflammation is associated in the acute phase with migration of neutrophils and leukocytes into the bowel. Faecal markers are non-invasive, low-cost, highly sensitive and specific tests for detecting local gastrointestinal inflammation12. Calprotectin is a protein derived directly from the neutrophil, and its concentration allows measurement of inflammation. It is therefore very useful for differentiating between inflammatory and functional processes. An increase in faecal calprotectin has been observed in the follow-up of patients with an acute episode of diverticulitis11, but there is no evidence to support its use as a predictor of recurrence or its correlation with worsening symptoms. Faecal calprotectin may also be useful in differentiating diverticular disease from IBS in patients with symptoms that are difficult to categorise.
Due to the lack of consensus and a standardized algorithm on the therapeutic management of patients with recurrent episodes of acute diverticulitis or persistent symptoms our group has initiated a prospective, multicentre project to answer these questions. The main objective of the DICRO project (Prospective and multicentre study on clinical-biological predictors of chronic diverticulitis of the colon -ClinicalTrials.gov Identifier: NCT04407793-) is to detect a prognostic factor of acute episodes recurrence in patients with chronic diverticulitis, with the aim of establishing a therapeutic algorithm to objectively determine which patients with chronic diverticulitis will need elective colonic resection in order to improve their QOL. We believe that the line of work we are proposing may have a great impact on chronic diverticular disease and will generate new projects in the future. The authors welcome other centres to join; please contact Dr Climent or Prof Biondo.
References
Schultz JK, Azhar N, Binda GA, Barbara G, Biondo S, Boermeester MA, et al. European Society of Coloproctology: guidelines for the management of diverticular disease of the colon. Colorectal Dis. 2020 Sep;22(S2):5–28
Comparato G, Di Mario F. Recurrent Diverticulitis. Journal of Clinical Gastroenterology. 2008 Nov;42(10):1130–4.
Trenti L, Kreisler E, Galvez A, Golda T, Frago R, Biondo S. Long-Term Evolution of Acute Colonic Diverticulitis After Successful Medical Treatment. World J Surg. 2015 Jan;39(1):266–74.
Lambrichts DPV, Bolkenstein HE, van der Does D, Dieleman D, Crolla RMPH, et al. Multicentre study of non-surgical management of diverticulitis with abscess formation. Journal of British Surgery. 2019 Mar; 106(4): 458-66.
Bolkenstein HE, de Wit GA, Consten ECJ, Van de Wall BJM, Broeders IAMJ, Draaisma WA. Cost-effectiveness analysis of a multicentre randomized clinical trial comparing surgery with conservative management for recurrent and ongoing diverticulitis (DIRECT trial). British Journal of Surgery. 2019 Feb 27;106(4):448–57.
Bolkenstein HE, Consten ECJ, van der Palen J, van de Wall BJM, Broeders IAMJ, Bemelman WA, et al. Long-term Outcome of Surgery Versus Conservative Management for Recurrent and Ongoing Complaints After an Episode of Diverticulitis: 5-year Follow-up Results of a Multicenter Randomized Controlled Trial (DIRECT-Trial). Annals of Surgery. 2019 Apr;269(4):612–20.
Biondo S. The diminishing role of surgery for acute diverticulitis. BJS 2019; 106:308-309.
Simpson J, Neal KR, Scholefield JH, Spiller RC. Patterns of pain in diverticular disease and the influence of acute diverticulitis: European Journal of Gastroenterology & Hepatology. 2003 Sep;15(9):1005–10.
Egger B, Peter MK, Candinas D. Persistent Symptoms After Elective Sigmoid Resection for Diverticulitis. Diseases of the Colon & Rectum. 2008 Jul;51(7):1044–8.
Oor JE, Atema JJ, Boermeester MA, Vrouenraets BC, Ünlü Ç. A Systematic Review of Complicated Diverticulitis in Post-Transplant Patients. J Gastrointest Surg. 2014 Nov;18(11):2038–46.
Tursi A, Brandimarte G, Elisei W, Giorgetti GM, Inchingolo CD, Aiello F. Faecal calprotectin in colonic diverticular disease: a case–control study. Int J Colorectal Dis. 2009 Jan;24(1):49–55.
Tibble JA, Sigthorsson G, Bridger S, Fagerhol MK, Bjarnason I. Surrogate markers of intestinal inflammation are predictive of relapse in patients with inflammatory bowel disease. Gastroenterology. 2000 Jul;119(1):15–22.



.png)





.jpg)




