BJS Academy>Cutting edge blog>Key questions in the...
Key questions in the diagnosis and management of appendicitis
James Ashcroft (@JamesAshcroftMD) Academic Clinical Fellow, Department of Surgery, Cambridge, UK; Salomone Di Saverio (@salo75) Consultant General and Colorectal Surgeon, Professor of Surgery, University of Insubria, Regione Lombardia, Italy; Justin Davies (@jdcamcolorectal) Consultant General and Colorectal Surgeon and Deputy Medical Director, Addenbrooke’s Hospital, Cambridge, UK.
31 May 2020
Guest Blog Colorectal
Related articles

PelvEx 2024
John T. Jenkins1, Paul Sutton2
1. Consultant Colorectal Surgeon
Chair of Surgery
Lead Complex & Recurrent Cancer Service,
St. Mark's Hospital, London
Imperial College, London
Surgeon to the Royal Household
2. Consultant Colorectal, Pelvic, and Peritoneal Surgeon
Colorectal and Peritoneal Oncology Centre
The Christie NHS Foundation Trust
Chair ACPGBI Advanced Malignancy Subcommittee
DOI: https://doi.org/10.58974/bjss/azbc052
PelvEx 2024 was hosted and organized in London by the ACPGBI Advanced Malignancy Subcommittee and UKPEN. The Royal Institution provided the perfect venue, blending history with excellent facilities which ensured the meeting was a tremendous success. Nearly 300 delegates attended from all over the world, with this year’s meeting having a truly multi-disciplinary programme.
The first day included sessions on “R0 resection – How important is it really”, “How much is too much in exenteration surgery”, and “Mastering morbidity”. In addition, sessions on the “Consequences of exenteration surgery” including patient and nursing experiences, as well as discussion about sex and intimacy, and the psychological consequences of surgery. The day finished with a “Consultants Corner- Grey Heads on Green Shoulders” session discussing a number of diverse challenges encountered at different stages in clinical practice .
The second day began with the inaugural trainee prize presentation session for the now coveted Brunschwig Prize. A number of high quality abstracts were received and the six best (linked below this blog) were invited to deliver oral presentations. The quality was exceptional. This session was followed by sessions on “Research progress” and “Surgical techniques”, followed by an afternoon where the “Oncologists have their say” culminating with a “Global MDT”. The conference was live streamed to China and recorded for posterity.

Bowel cancer is not just a disease of older people
Katherine Goodall is a general surgical registrar from Queensland Australia
A young surgeon’s experience as a patient with bowel cancer
If you ask any clinician, becoming a patient is an unusual experience. When you couple that with the naivety of youth, embracing the role of a patient is particularly challenging.
As part of surgical training, and even in medical school, there are specific red flags that are taught to all of us. ‘Bowel habit change’ and ‘per rectal bleeding’ are not a great combination. We are also taught that we when we hear hoof beats, we should think horses, not zebras. So when I developed these symptoms I just assumed that I probably had a benign cause of bleeding. I assumed this for six weeks while I worked in a high volume liver and kidney transplant unit until I decided it was bothersome. I picked up the phone to one of my mentors, a colorectal surgeon. She subsequently performed my low anterior resection.
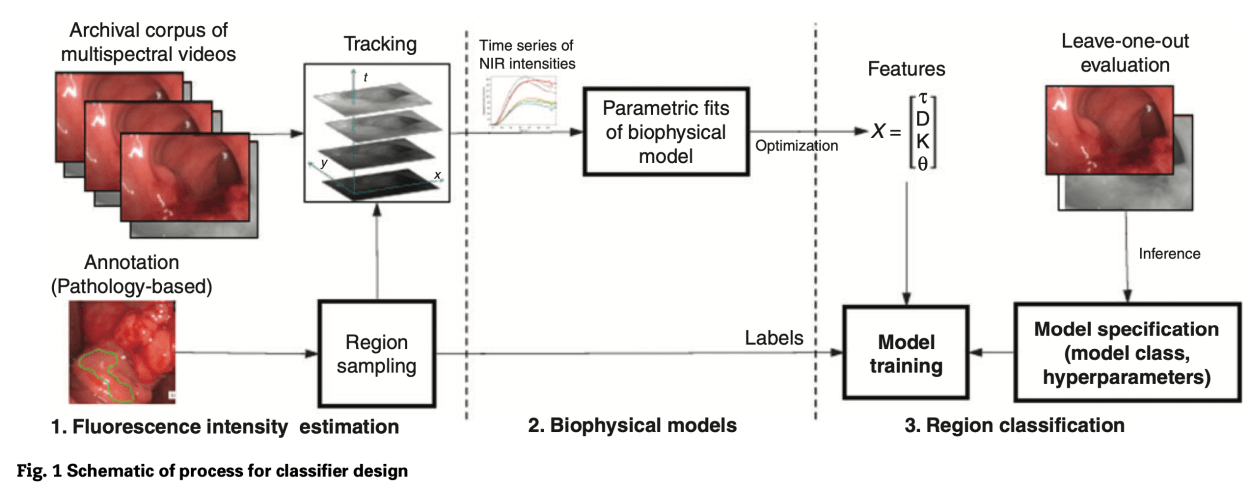
Guest blog: 21st century surgery is digital
Ronan Cahill, Digital Surgery Unit, Mater Misericordiae University Hospital, Dublin, Ireland and UCD Centre for Precision Surgery, Dublin, Ireland.
Niall Hardy, UCD Centre for Precision Surgery, Dublin, Ireland.
Pol MacAonghusa, IBM Research, Dublin, Ireland.
Twitter @matersurgery Email: ronan.cahill@ucd.ie
Copied!
Connect

Copyright © 2026 River Valley Technologies Limited. All rights reserved.



.png)





.jpg)



