What’s wrong?
Do you want me to deflate the pneumoperitoneum?
My surgeon stops what he’s doing and just looks at me expectantly. I hadn’t said anything to him, nor had I really clocked my own discomfort as something about my patient’s physiology didn’t quite fit with the usual Feng Sui pattern I was expecting.
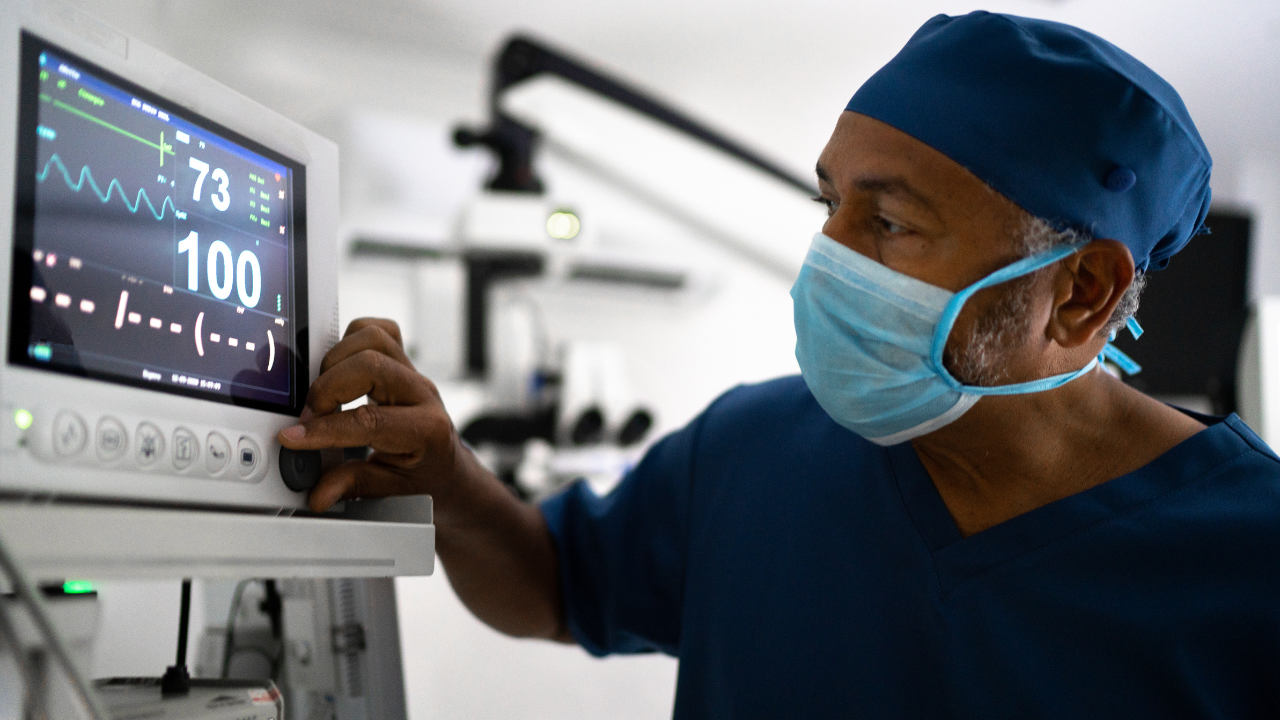
Invariably he was right, my endotracheal tube had displaced just a little and caused some partial obstruction at the carina, my end tidal CO2 trace wasn’t quite as normal as it should be, while the airway pressures were just a little higher than they had been. It was quickly resolved by pulling it back a touch, all the patterns fell back into place and order was restored. I went back to my relaxed exterior while obviously maintaining my usual cat-like observation that years of experience has made an automatic reflex.
This encounter made me think about how we respond to subtle signals from each other. There was clearly something in my posture, the way I watched the monitor, the way I went quiet in a non-relaxed kind of way that set his alarm bells ringing. It didn’t fit his expected pattern. He almost noticed the problem before I did and went into a well-practised drill to make things safe and remove the intra-abdominal pressure that could be adding to my problem.
My Tuesday surgeon and I have worked together since we were both appointed as consultants eighteen years ago, we have become comfortable with each other and highly attuned to when the other is struggling. I was discussing this with one of my other anaesthetic colleagues who talked about their surgeon going quiet, a change in the noise of the suction, the changing tone of the surgeon’s interaction with the scrub nurse.
In my opinion, the operating theatre remains one of the best places to study safety, human interaction and non-technical skills. There is nowhere else where two doctors from different specialties work together in such close proximity, in differing but interweaving roles, where the patient’s wellbeing is dependent on great communication and collaboration.
I like watching my surgeons operate. It gives me an idea of how things are going and allows me to anticipate any issues I might have. I always have one of the laparoscopy screens facing me and teach my residents that it’s important we know what the surgeons are doing at any point. In obstetrics we shouldn’t have to wait for the surgeon to tell us that the uterus is hypotonic or if there is bleeding, we should see it ourselves. Our surgeons might be task focused and forget to tell us, which shouldn’t delay us getting on resuscitating the patient, giving tranexamic acid and whatever else the situation demands.
I think surgeons understand less about what we do, probably because we usually anaesthetise behind the closed doors of the anaesthetic room, or if in theatre they’re rarely in the room at that point. I think this changed somewhat after COVID redeployment when many of the surgical residents worked on the intensive care unit. This culminated a couple of years ago when my patient started coughing on the ventilator and instead of the usual “THE PATIENT IS WAKING UP” I got a very calm “Excuse me Helgi, I think the rocuronium has worn off and the patient isn’t synchronising with the ventilator, could you give him some more?”
Let’s imagine every surgeon did six months of anaesthesia in their training and every anaesthetist reciprocated with six months of surgery. Would our interactions change with the increased understanding? And if so, what would the changes be?
If we look at technical skills, I think we anaesthetists would benefit from improved suturing and practical skills and a greater understanding of how tissue layers form and how it translates to the haptic feedback we get when doing epidurals or nerve blocks. However, I think the greatest benefit for the surgeon/anaesthetist relationship would be a better understanding of the different pressures on a surgeon. We generally only have to be in one place at a time, whereas when I call the surgical registrar to do an appendicectomy on my emergency list the ward round may be delayed, the patient waiting for surgical assessment in the emergency department waits longer, or a discharge decision gets delayed. A lot of these decisions still need to be made though, and invariably the surgeon ends up taking calls when they’re trying to focus on operating. Should this change, with intraoperative decision-making separated from the general on-call? Almost certainly, but in the meanwhile, we need to give our surgeons a bit of slack when they’re late to the team brief.
I asked the surgeons I’m working with today what they think they would learn from an anaesthetic placement. They responded enthusiastically with improved technical skills, with central venous lines, ultrasound and general practical procedures, pain management, but even more so with their improved understanding of perioperative medicine and general physiology. They were a little worried that their residents wouldn’t want to come back to surgery, having seen the green fields and clover on this side of the Blood-Brain Barrier.
The relationship between anaesthetist and surgeon is like a marriage. We are at our absolute best when we cooperate, understand each other’s idiosyncrasies and step up when the other person is having difficulties. Our patients benefit the most when we understand the risk posed by both sides of the Barrier, making our decisions together in their best interests.
…and coffee.





.png)





.jpg)




