BJS Academy>Cutting edge blog>Guest blog: Keyhole ...
Guest blog: Keyhole versus open surgery for oesophageal cancer
B. P. Müller-Stich, P. Probst, H. Nienhüser, S. Fazeli, J. Senft, E. Kalkum, P. Heger, R. Warschkow, F. Nickel, A.T. Billeter, P. P. Grimminger, C. Gutschow, T. S. Dabakuyo-Yonli, G. Piessen, M. Paireder, S. F. Schoppmann, D. L. van der Peet, M. A. Cuesta, P. van der Sluis, R. van Hillegersberg, A. H. Hölscher, M. K. Diener, T. Schmidt
28 September 2021
Guest Blog Upper GI
Related articles

Management of Crohn’s Disease. The shiny medical sports car or the worn out surgical banger?
Professor Steven R Brown, Sheffield Teaching Hospitals. Based on the BJS Lecture at ACPGBI 2020
Professor Steven R Brown, Sheffield Teaching Hospitals.
Based on the BJS Lecture at ACPGBI 2020
A success story

Visual abstract: Merged SLEEVEPASS and SM-BOSS trials
Laparoscopic Roux-en-Y gastric bypass versus laparoscopic sleeve gastrectomy: 5-year outcomes of merged data from two randomized clinical trials (SLEEVEPASS and SM-BOSS)
Recently published as open access in BJS, the 5-year results of the merged Finnish SLEEVEPASS and Swiss SM-BOSS randomised controlled trials comparing laparoscopic sleeve gastrectomy with laparoscopic Roux-en-Y gastric bypass shows that Roux-en-Y led to greater weight loss and better control of hypertension than sleeve gastrectomy, with no difference in outcomes for type 2 diabetes, obstructive sleep apnoea, or quality of life. More details can be found in the paper.
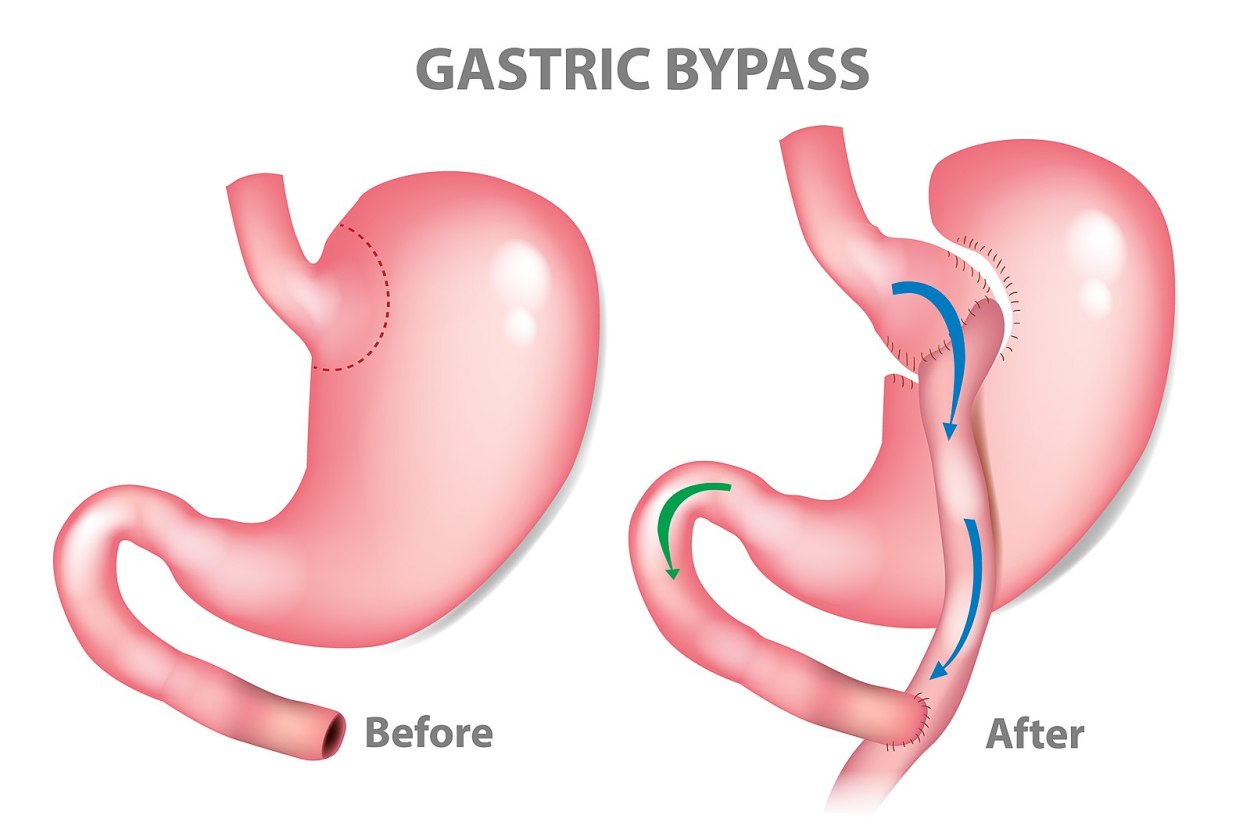
Guest blog: Bariatric Surgery – the safe solution to the metabolic pandemic
A G N Robertson (Twitter: @robertson_a), T Wiggins (@TomWiggins23), F P Robertson, L Huppler (@LucyLucyHuppler), B Doleman, E M Harrison (@ewenharrison), M Hollyman (@misshollyman), R Welbourn
Obesity is the preventable and reversible disease of our lifetime. It is a worldwide health, economic and environmental problem in need of urgent and essential attention, and it has become clear that the world needs more than the traditional recommendations to survive this metabolic pandemic. The traditional advice has been acknowledged for centuries and even more so since the worldwide prevalence of obesity nearly tripled between 1975 and 20161. These lifestyle recommendations include physical exercise, less high calorific food content, balanced meals, optimising portion size, intermittent fasting and so on; we all know them. However, the human race is still falling short of tackling the major public health concern that this disease threatens to be.
Bariatric or weight loss surgery is a surgical sub-speciality which has been evolving since the first procedures of this type in the mid 20th century. Its development has led to the most effective method to achieve long-term weight loss, as well as the additional health benefits weight loss offers as a by-product. However, accessibility to this specialist treatment is limited with only 1% of eligible patients going on to receive bariatric surgery.2Reasons for this limited access are multifactorial, however a considerable factor is thought to be concerns regarding the perceived risks of weight-loss surgery from patients across all populations. We should therefore aim to give our patients the most up to date worldwide risk of mortality of these potentially life-saving procedures.
This month in the BJS, we’ve published the largest meta-analysis asking this question to date – and the findings are pivotal at providing a unanimous international statistic on this discussion. We’ve looked at perioperative mortality rates (inpatient, 30 day and 90 day mortality) of a range of bariatric procedures to include laparoscopic adjustable gastric band (LAGB), sleeve gastrectomy (SG), Laparoscopic Roux-en-Y gastric bypass (LRYGB), one-anastomosis gastric bypass (OAGB), biliopancreatic diversion/duodenal switch (BPD-DS) and other malabsorptive procedures. We’ve included 58 studies in our meta-analysis which has given us information on roughly 3.6 million patients over a 6-year period from worldwide practice. Multiple sources for data were used including administrative datasets, bariatric surgery registries, large scale case series as well as randomised controlled trials (RCTs).
Copied!
Connect

Copyright © 2026 River Valley Technologies Limited. All rights reserved.



.png)





.jpg)



